Clearance, Kt/V, and Concentration in a Reverse Flow Dialyser
Instantaneous Clearance: Kd
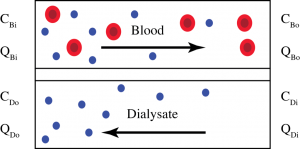
CBi, and CBo are the concentration of solute in the blood at the input and output of the dialyser. CDi and CDo are the concentration of solute in the dialysate at the input and output. QBi, QBo, QDi, and QDo are the flow rates at the inputs and outputs. The volume of blood completely cleared of a given solute per unit time, K, is found by the following formula. which is the difference between the mass flow rate or removal rate (mg/min.) divided by the input concentration (mg/mL) giving a volumetric clearance rate (mL/min.).
If we assume that QBi = QBo and rearranging the terms we get the next equation. This assumption simply means that the volume of the filtrate (the solute that passes through the filter) is much smaller than the volume of the blood passing through the dialyser (e.g. there is no ultrafiltration of water through the membrane)
Note: the dimensionless quantity (1-CBo/CBi) is called the extraction ratio. It can be seen that if all of the solute is removed and CBo = 0 then the dialysis rate is equal to the the flow rate of the blood through the dialyser (K = QBi). If none of the solute is removed and CBo = CBi then the dialysis rate is equal to zero (K = 0).
Mean (integrated) Clearance
For dialysis, and the kidney itself, the removal rate is a linear function of concentration, the first order differential equation is given below.
Where C is the concentration and k is the elimination constant expressed as a fraction per unit time.
Multiplying by the total blood volume, V (aka urea volume of distribution) gives the solute removal rate over concentration (the clearance K).
Integrating this equation leads to…
and solving for k, the elimination constant…
and because K = kV we arrive at the relation ship between clearance, K, and the change in solute concentration.
This shows the exponential reduction of solute concentration over time with a time constant of t= V/K.
Clinicians use a target of Kt/V ≥ 1.2.
Of course, it is really much more complicated than this. This is the standard Kt/V, there is also a normalized Kt/V which takes into account that according to [Kaysen 1997] and others urea is a poor representative of retained toxic solutes and effective toxin clearance. The widely accepted measure of dialysis adequacy is the Kt/Vurea. It is recommended that patients with low residual kidney function under going dialysis three times a week need a 1.2 at a minimum and a goal of 1.4 for this measure. It is important to remember that while urea clearance is an accepted metric for dialysis efficacy, there are other solutes, such as creatinine, that do not move across the erythrocyte membrane very quickly so creatinine clearance is not correlated to urea clearance.
In addition, this all relates to reverse flow systems and modifications or approximations will need to be considered to find similar equations for a closed dialysate system.
Kaysen GA, Stevenson FT, Depner TA. Determinants of albumin concentration in hemodialysis patients. AM J Kidney DIs 1997:29(5); 658-668.
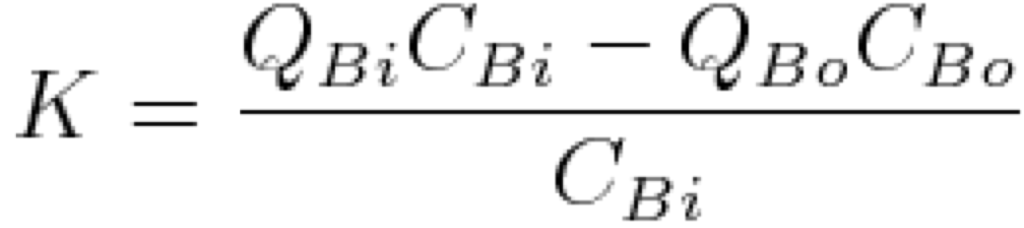
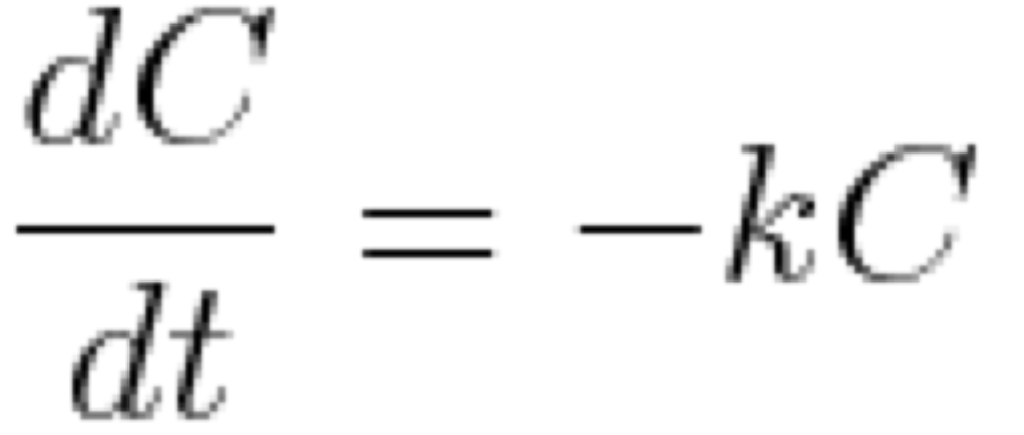
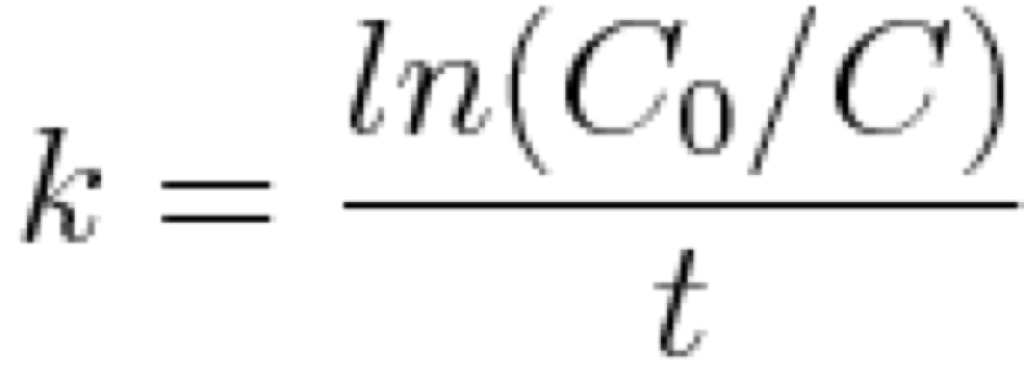

I keep coming back to this post to look up the urea reduction level that corresponds to the target KT/V values and I always have to calculate it. So I’m putting it in this comment:
KT/V = 1.2 is a reduction to 30%
KT/V = 1.4 is a reduction to 24%