Heart on a Chip (Healy Group)
Kevin Healy is a Phase I and Phase II awardee of the NIH Tissue Chip initiative.
The goal of this initiative is to create ‘mini-organs’ ‘organs-on-a-chip’ ’tissue chips’ or ‘microphysiological systems’ (MPS) for higher throughput and more reliable drug discovery. The effort is also motivated by the failure of recent animal models to predict drug efficacy in human trials (discussed in Esch, et al., Nat Rev Drug Discov, 2015).
Background:
- Average drug launch is 5 billion USD and preclinical development and clinical studies account for 63% and 32% of this cost, respectively.
- Inter-species differences in ion channels, biological pathways, and pharmacokinetic properties mean animal models often fail to fully recapitulate human physiology.
- Patient-specific human induced pluripotent stem cells (hiPSCs) for personalized drug
screens? - Static 3D tissue constructs do not provide microcirculation like the vasculature, which
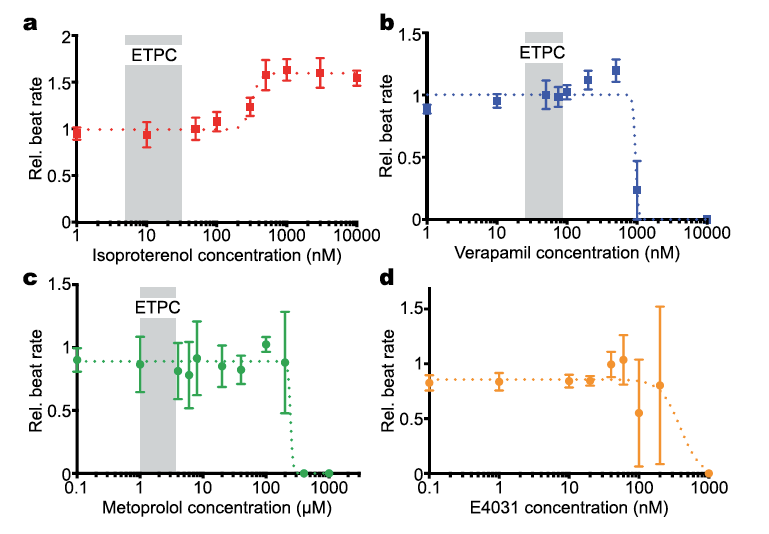
includes the capability to continuously exchange the nutrients, constant exposure of the tissue to fresh drug in the plasma, and convective-diffusive oxygen/nutrient transport. - This is an attempt to make appropriate biophysical tissue architecture and ‘‘tissue-like’’ drug gradients for accurate prediction of the cardiotoxicity of drugs.
Results:
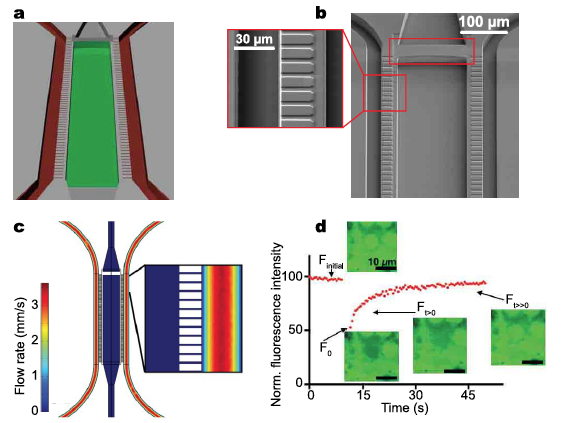 Figure 1: Central channel for cells. PDMS walls with 2 um x 2 um x 30 um channels. Exchanges nutrients but no convection. Model of the ‘vasculature.’
Figure 1: Central channel for cells. PDMS walls with 2 um x 2 um x 30 um channels. Exchanges nutrients but no convection. Model of the ‘vasculature.’
- Source of hiPSCs?
- Loaded into device after partial differentiation to avoid excessive buildup of ECM.
- Spontaneous beating at 55-80 bpm. See movie here.